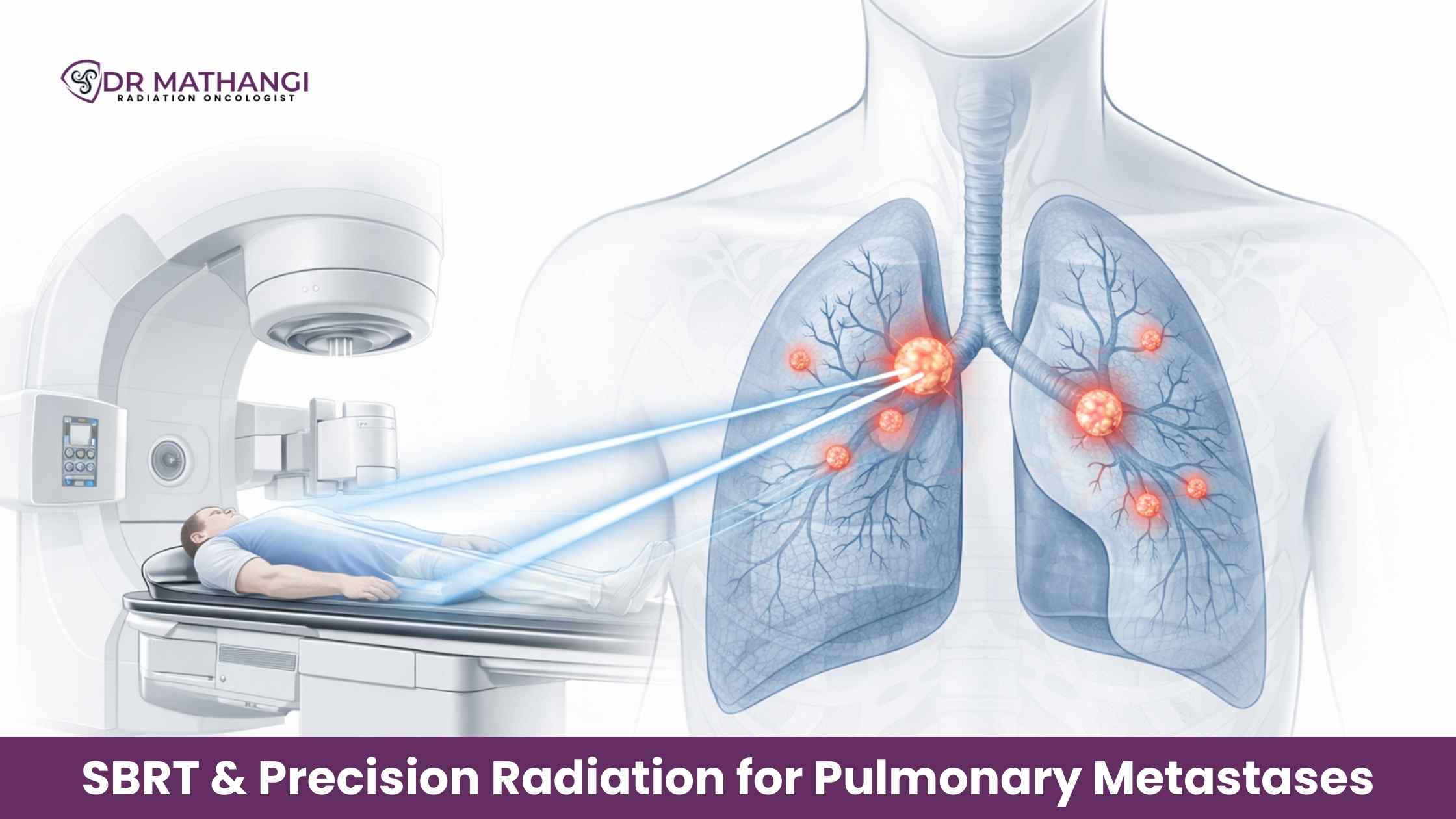
Nearly 30–50% of patients with advanced solid tumors may develop lung metastases during the course of their disease. SBRT & Precision Radiation for Pulmonary Metastases has transformed outcomes for many of these patients by offering highly targeted, non-invasive treatment that can control disease with minimal damage to healthy lung tissue. Under the leadership of Dr Mathangi J, Senior Consultant & In-charge – Radiation Oncology at Gleneagles Cancer Institute, Bangalore, this advanced approach has redefined hope for patients across South India and North India.
Pulmonary metastases occur when cancer cells from a primary tumor—such as breast, colorectal, kidney, or head and neck cancers—spread to the lungs. These secondary tumors can appear as solitary nodules or as multiple pulmonary metastases scattered throughout the lung fields.
They may involve the pulmonary parenchymal metastases, meaning the functional lung tissue itself, and in some cases may present as cavitating pulmonary metastases, where the tumor forms a hollowed-out cavity. Another clinical scenario includes lung to lung metastasis, where cancer originating in one lung spreads to the other.
Each presentation requires a highly individualized pulmonary metastases treatment strategy, and this is where precision radiation becomes crucial.
Stereotactic ablative body radiotherapy (SBRT) delivers very high doses of radiation with sub-millimeter precision over fewer sessions. It is particularly effective for:
Unlike conventional radiation, SBRT focuses on the tumor with remarkable accuracy, sparing surrounding lung parenchyma. For patients with multiple pulmonary metastases, carefully planned SBRT may still be an option depending on disease burden and location.
Precision radiation integrates imaging, motion management, and advanced delivery platforms. At Dr Mathangi’s center, technologies such as Image-Guided Radiotherapy (IGRT), RapidArc, and gated techniques ensure radiation tracks tumor motion during breathing.
This level of accuracy is particularly critical in pulmonary parenchymal metastases, where preserving lung function is paramount.
Dr Mathangi J is a Senior Radiation Oncologist with over 20 years of experience and more than 12,000 successfully treated patients. She completed her DMRT at Madras Medical College and her DNB at Apollo Cancer Specialty Hospital, Chennai. Her advanced training in Stereotactic techniques (SRS/SBRT) from Klinikum Frankfurt (Oder), Germany, IGRT/RapidArc from Copenhagen University Hospital, Denmark, and IORT training have positioned her among India’s leading experts in precision oncology.
She currently heads the radiation oncology department and serves as Director of Fellowship in Advanced Radiotherapy techniques affiliated with RGUHS. Notably, she was instrumental in installing the Asia Pacific’s first TrueBeam STx machine.
When facing something as complex as lung to lung metastasis or cavitating pulmonary metastases, experience is not optional—it is decisive.
Cancers that frequently spread to the lungs include:
Radiation therapy plays a vital role either as definitive, consolidative, or palliative treatment in many of these conditions.
| Feature | Conventional RT | SBRT |
|---|---|---|
| Number of Sessions | 20–30 | 3–5 |
| Precision | Moderate | Sub-millimeter accuracy |
| Dose Per Fraction | Lower | Very high |
| Impact On Healthy Lung | Broader exposure | Highly targeted |
For carefully selected patients with multiple pulmonary metastases, SBRT can achieve local control rates exceeding 80–90% in many clinical studies.
The process is structured, precise, and patient-centric.
Delaying therapy in pulmonary metastases may allow progression from a limited oligometastatic state to widespread disease. Early intervention with SBRT can convert a potentially life-limiting scenario into a controlled condition.
Many patients underestimate symptoms until they experience breathlessness or persistent cough. By then, lesions may have grown or multiplied. Acting early under the guidance of an expert like Dr Mathangi can preserve lung function and extend survival.
Cavitating pulmonary metastases require careful radiation planning because the structural integrity of lung tissue is altered. SBRT’s precise targeting minimizes surrounding damage while delivering ablative doses directly to the tumor cavity margins.
Similarly, lung to lung metastasis demands strategic evaluation to differentiate new primaries from metastatic deposits. Precision imaging and biopsy correlation guide treatment planning.
Patients across India travel to Bangalore seeking her expertise because precision is not just about machines—it is about judgment, planning, and execution.
Dr Mathangi J is a Senior Consultant & In-charge – Radiation Oncology at Gleneagles Cancer Institute, Bangalore. She specializes in Head and Neck Cancers, Prostate Cancers, Brain Tumors, Lung Cancers, and Women Cancers including Breast, Cervix, and Endometrium. Her commitment to academic excellence and patient-centered care positions her as a trusted authority in advanced radiation therapy.
If you or a loved one has been diagnosed with pulmonary metastases, waiting can mean losing the window where precision therapy offers maximum benefit. SBRT & Precision Radiation for Pulmonary Metastases is not merely a treatment option—it can be a turning point.
To book an appointment, submit your contact information at https://drmathangi.com/contact/. Dr Mathangi’s team will schedule your consultation and guide you through the next steps toward personalized, precision-driven cancer care.