Nearly 60–90% of oral cancer patients undergoing traditional radiation therapy experience dry mouth after radiation treatment, a condition medically known as xerostomia. However, modern advancements in radiation therapy salivary gland preservation have dramatically changed this reality, allowing patients to undergo effective cancer treatment while maintaining essential gland function.
Under the expertise of Dr Mathangi J, Senior Consultant & In-charge – Radiation Oncology, patients benefit from cutting-edge techniques designed not just to treat cancer, but to preserve their dignity, comfort, and quality of life radiation therapy outcomes.
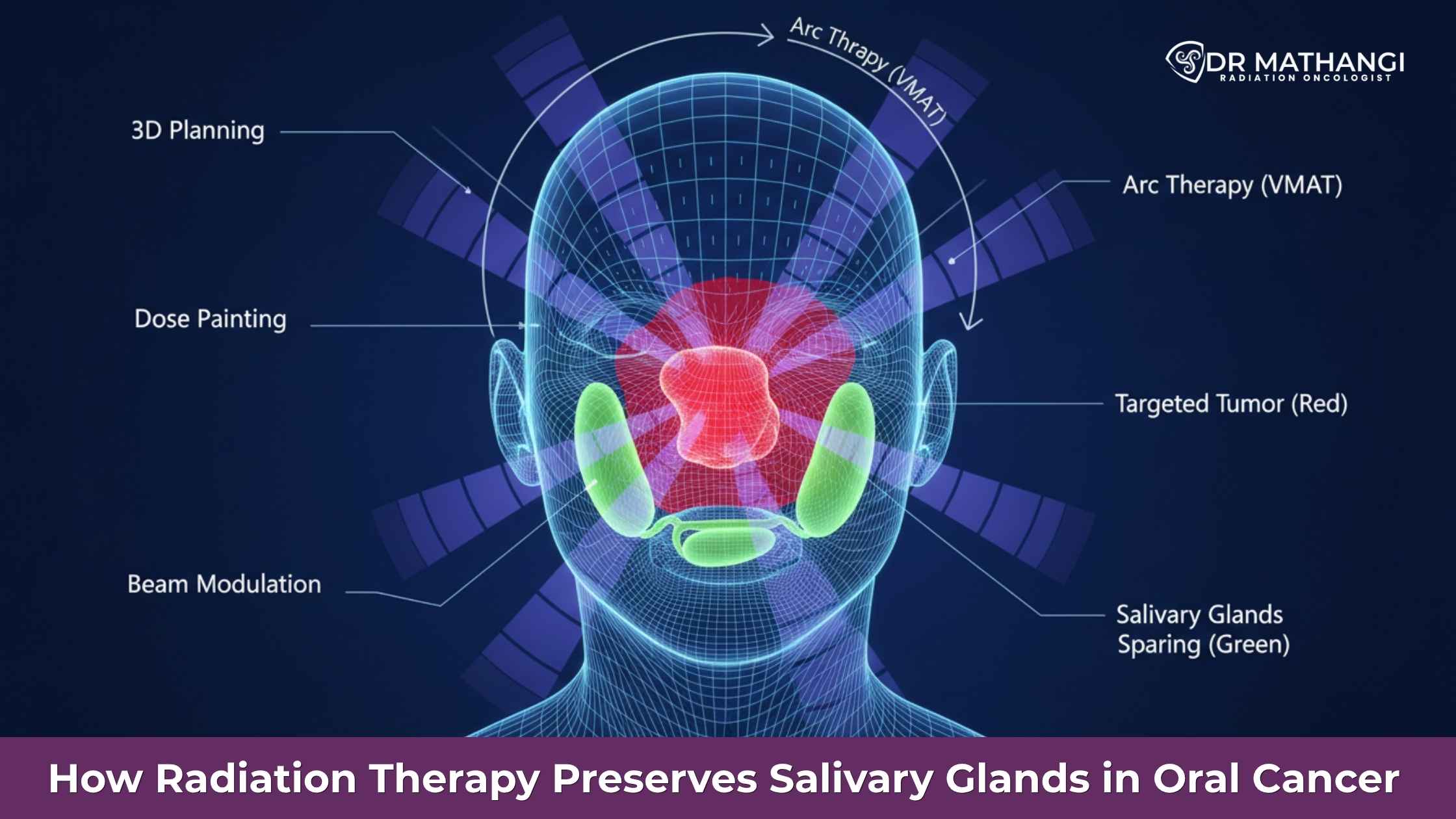
Radiation therapy salivary gland preservation refers to advanced radiotherapy methods that specifically target cancer cells while minimizing radiation exposure to the salivary glands. This helps reduce complications like dryness, swallowing difficulties, and speech issues.
Traditional radiation often affected surrounding tissues indiscriminately. Today, precision-based technologies ensure:
This shift represents a major leap forward in salivary gland protection radiotherapy.
Xerostomia radiation therapy prevention is crucial because saliva plays a vital role in oral health, digestion, and infection control. Without adequate saliva, patients may face long-term complications.
Problems caused by untreated xerostomia include:
By prioritizing gland preservation, Dr Mathangi ensures that treatment goes beyond survival — it supports a patient’s overall well-being.
Radiotherapy side effects oral cancer patients experience can vary depending on treatment intensity and technique. However, common effects include:
| Side Effect | Description |
|---|---|
| Dry mouth | Reduced saliva production leading to discomfort |
| Mucositis | Inflammation and sores in the mouth |
| Taste changes | Altered or reduced sense of taste |
| Difficulty swallowing | Due to tissue inflammation |
Advanced gland sparing radiation therapy techniques significantly reduce these complications.
Gland sparing radiation therapy techniques use sophisticated imaging and delivery systems to avoid unnecessary radiation exposure to the salivary glands.
Dr Mathangi employs globally recognized technologies such as:
These methods ensure optimal salivary gland protection radiotherapy while effectively eliminating cancer cells.
Quality of life radiation therapy outcomes are now a central focus in oncology. Patients are no longer expected to endure severe side effects as a trade-off for survival.
With advanced care, patients benefit from:
This holistic approach is at the core of Dr Mathangi’s treatment philosophy.
Dr Mathangi J is a highly respected name in radiation oncology, with over 20 years of experience and more than 12,000 successfully treated patients. She leads the Radiation Oncology department at Gleneagles Cancer Institute, Bangalore.
Her expertise includes:
She has received advanced international training in:
She is also recognized for installing the Asia Pacific’s first TrueBeam STx Machine, a breakthrough in precision radiotherapy.
Choosing Dr Mathangi means choosing:
Radiation therapy is a key treatment modality for multiple cancers, including:
This wide scope highlights the importance of expert-led radiation oncology care.
Without proper radiation therapy salivary gland preservation, patients may experience lifelong complications that affect daily living.
These include:
This is why choosing the right specialist and technology is critical — delaying or opting for outdated methods can significantly impact recovery.
If you or your loved one is facing oral cancer, early intervention with advanced techniques can make a life-changing difference.
To consult Dr Mathangi:
Taking action today ensures access to the most advanced xerostomia radiation therapy prevention and treatment protocols available.
Dr Mathangi J is a Senior Radiation Oncologist and In-charge at Gleneagles Cancer Institute, Bangalore. With over two decades of experience, she specializes in advanced radiotherapy techniques that prioritize both cancer control and patient comfort. Her leadership in innovation and commitment to excellence make her one of the most trusted names in oncology.